Covered by OHIP?
Most services are covered by the Ontario Health Insurance Plan (OHIP)
Waiting Time
Your timeframe depends on the type of procedure.
OHIP Covered Services
Most services are covered by the Ontario Health Insurance Plan (OHIP)
WILDERMAN MEDICAL CLINIC
What is spinal stenosis?
The spine is an important series of bones that helps support the body and protect the nerves that pass within it (Comer et al., 2022). The medical term “stenosis” means “the narrowing of”, and indicates that there is an issue with the width or length of a particular body part.
As such, spinal stenosis is the abnormal narrowing of the spine, typically occurring in the lower back, though it may occur in the neck as well. This change in space found within the spine causes pressure, irritation, or damage to the nerves that pass through the narrowed portion of the spinal canal.
This may lead to chronic and debilitating pain, shooting pain, numbness and/or weakness below the area affected, balance issues, and a loss of muscle control.
Spinal stenosis is a disorder that worsens over time and may not be noticed until the narrowing is severe enough for symptoms to develop.
Anatomy of the spine
The spine is what allows us to stand up and support our own weight throughout the day (TeachMeAnatomy, 2022).
It is composed of 33 bones, called vertebrae, which are divided into 5 sections: the cervical section, which has 7 vertebrae; the thoracic section, which has 12 vertebrae; the lumbar section, composed of 5 vertebrae; the sacrum section, which has another 5 vertebrae; and the coccyx, which is composed of 5 fused vertebrae.
Each vertebra is identified by its section and the order in which it is found, from top to bottom. There is a cushion of cartilage between each vertebra, which allows the spine to move smoothly.
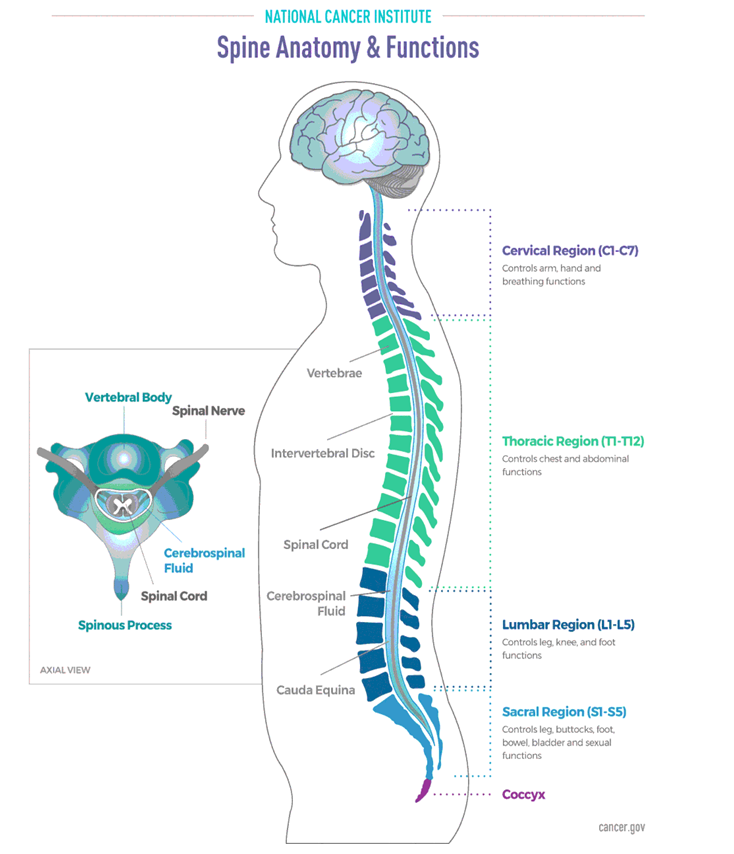
When viewed from the side, the spine has a very slight ‘S’ shape.
Each vertebra has a canal at its center, which allows the nerves to pass through the spine, well protected by the bones surrounding them.
The nerves are bathed in a fluid called cerebrospinal fluid, which flows throughout the spine and brain to maintain the nerves.
Symptoms
Spinal stenosis may be asymptomatic (without symptoms) or be accompanied by some or all of the below symptoms. The type of symptoms experienced depends on where the narrowing is and the degree of severity.
Common symptoms of spinal stenosis include:
• Pain
• Muscle weakness
• Numbness
• Balance issues
If the spinal stenosis is at the cervical (neck) level:
• Neck pain and/or tension
• Numbness that affects the arms, legs, hands, or feet
• Muscle weakness
• Trouble making precise movements
• Balance issues
• Loss of bladder or bowel control
If the narrowing is found at the thoracic (chest and/or abdomen) level:
• Pain
• Numbness
• Muscle weakness
• Balance issues
And if the issue is at the lumbar (lower back) level:
• Pain
• Sciatica: a shooting pain that goes from the buttock down toward the foot
• Weakness in the legs and feet
• Numbness
The pain associated with spinal stenosis is described as a burning sensation, a dull ache, tenderness, or an electric shock. This pain may disappear or lessen when in different positions but comes back or increases when standing or walking for long periods.
Risk factors
While spinal stenosis can happen to anyone, research has identified several risk factors (Wan et al., 2023). Some of these can be managed, while others cannot.
Risk factors for spinal stenosis include:
• Genetic predisposition for spinal disorders
• Smoking – with the associated risk of spinal stenosis lowering with smoking cessation
• Low-income background: a lack of consistent nutrition and medical access will impact the overall health of a person
• Having low physical activity habits
• Chronic and frequent activities that bend the neck forward such as the use of mobile phones, laptops, tablets, and improperly set up workstations
• Chronic and improper lifting habits
• Lack of core strength
• Diabetes: the risk is higher if diabetes is not well controlled (Asadian et al., 2016)
• Diet high in fat and processed foods (Ruggiero et al., 2022)
• Past traumatic spinal injury
• Spinal surgeries
• Osteoporosis
• Scoliosis
• Being over 50 years old: risk increases with age
Causes
There are numerous causes for spinal stenosis, some are a result of unhealthy habits, and others are due to other disorders (Raja et al., 2022; Melancia et al., 2014).
These causes are divided into two categories: causes with a genetic component and other causes.
Genetically influenced causes:
• Congenital malformations of the spine and/or spinal canal
• Osteoporosis
• Scoliosis
• Kyphosis: the gradual rounding of the back, often seen in seniors
• Morquio syndrome: a genetic disorder that changes how the body processes specific types of sugars
• Spinal osseous exostosis: an abnormal bone growth on top of another bone
Genetic causes are responsible for an estimated 9% of spinal stenosis cases.
Other causes:
• Spinal trauma, such as car or motorcycle accidents or falls
• Spinal disc hernias
• Arthritis
• Cushing disease: a condition in which the body produces too much cortisol
• Calcium metabolism issues
• Chronic inflammatory disorders
• Spinal infections
Diagnosis
In order to diagnose spinal stenosis, a doctor will ask you to explain your symptoms, how long you’ve been having them, and if you have any risk factors that may increase your chances of developing the condition.
After that, a physical exam will be done, assessing your spine, reflexes, vestibular system, muscle strength, and sensation in your arms and/or legs.
To rule out other disorders and further confirm the degree of spinal stenosis, your doctor may ask for additional tests such as:
• Glasgow lumbar spinal stenosis scale (Bradley et al., 2023)
• Spinal MRI, CT scan, and/or X-rays
• Nerve conduction testing
Treatment
The treatment for spinal stenosis depends on the location and severity of the stenosis; however, there is a consensus on the best approach to any kind of spinal stenosis (Comer et al., 2022).
If the symptoms are minimal:
• At-home physiotherapy
• Lifestyle changes, such as smoking cessation, dietary changes, and exercise to reduce possible risk factors
• Occupational therapy to improve ergonomics at home and/or work
If the symptoms are moderate or if at-home physiotherapy is not possible:
• Supervised physiotherapy for the core
• Mobility devices: cane, walker, and/or wheelchair
• Braces
• Psychotherapy
If the pain is consistent, moderate to severe, and/or an infection or inflammation is believed to be involved:
• Pain management treatment plan
• Anti-inflammatory medication
• Antibacterial or antiviral medication
• Epidural injections: injections of specific types of medications, usually for pain, into the space around the spinal cord. This should be considered if the pain is mostly felt on a single side and is hard to manage otherwise.
If the symptoms are severe, debilitating, and/or do not respond to the above treatments:
• Decompression surgery
• Spinal injections
• Spinal disc fusion: a surgery that combines (fuses) at least two discs together to stabilize the spine
If another disorder is involved in your spinal stenosis, your doctor will provide additional treatments to address any additional issues.
Spinal stenosis as a risk factor for other disorders
Kobayashi et al. (2022) found that the presence of spinal stenosis was a risk factor for the development of dementia in seniors.
Spinal stenosis is considered a risk factor for the following disorders:
• Cauda equina syndrome (CES): a rare and serious condition where the caudal nerves, found in the lumbar spine, are compressed or damaged and can lead to chronic incontinence and paralysis.
• Sleep disorders: The pain associated with spinal stenosis can lead to insomnia and other sleep disorders.
• Metabolic syndrome: the sudden appearance of several metabolic disorders within a short amount of time. These disorders may include diabetes, high blood pressure, increased weight gain, high cholesterol, and/or insulin resistance (Ono et al., 2022).
In many cases, the treatment of spinal stenosis will reduce the risks of developing other disorders.
What do we do at WMC?
At the Wilderman Medical Clinic, we offer a variety of interventional and non-interventional pain management options, including:
Interventional pain management for spinal stenosis:
• Caudal steroid epidural injections for spinal stenosis
• Lumbar steroid epidural injections for spinal stenosis
Non-interventional pain management for osteoarthritis of the thoracic facet joints:
• Psychotherapy
• Kinesiology education sessions
Reference
Asadian, L., Haddadi, K., Aarabi, M., & Zare, A. (2016). Diabetes Mellitus, a New Risk Factor for Lumbar
Spinal Stenosis: A Case–Control Study. Clinical Medicine Insights, 9, CMED.S39035.
https://doi.org/10.4137/cmed.s39035
Bradley, R., Kumar, A., & Barrett, C. (2023). The glasgow lumbar spinal stenosis scale: an individualised
measurement formula for the radiological assessment of lumbar spinal stenosis. British Journal of
Neurosurgery, 37(1), 63–66. https://doi.org/10.1080/02688697.2021.1958148
Comer, C., Ammendolia, C., Battié, M. C., Bussières, A., Fairbank, J., Haig, A. J., Melloh, M., Redmond, A.
C., Schneider, M., Standaert, C. J., Tomkins-Lane, C., Williamson, E., & An, H. S. (2022). Consensus on a
standardised treatment pathway algorithm for lumbar spinal stenosis: an international Delphi study.
BMC Musculoskeletal Disorders, 23(1). https://doi.org/10.1186/s12891-022-05485-5
Kalichman, L., Cole, R. N., Kim, D. H., Li, L., Suri, P., Guermazi, A., & Hunter, D. J. (2009). Spinal stenosis
prevalence and association with symptoms: the Framingham Study. The Spine Journal, 9(7), 545–550.
https://doi.org/10.1016/j.spinee.2009.03.005
Kobayashi, H., Tominaga, R., Otani, K., Sekiguchi, M., Nikaido, T., Watanabe, K., Kato, K., Yabuki, S., &
Konno, S. (2022). Lumbar spinal stenosis is a risk factor for the development of dementia: locomotive
syndrome and health outcomes in the Aizu cohort study. European Spine Journal, 32(2), 488–494.
https://doi.org/10.1007/s00586-022-07318-4
Melancia, J. L., Francisco, A. F., & Antunes, J. L. (2014). Spinal stenosis. Handbook of Clinical Neurology,
119, 541–549. https://doi.org/10.1016/B978-0-7020-4086-3.00035-7
Ono, R., Takegami, M., Yamamoto, Y., Yamazaki, S., Otani, K., Sekiguchi, M., Konno, S., Kikuchi, S., &
Fukuhara, S. (2022). Impact of lumbar spinal stenosis on metabolic syndrome incidence in community
dwelling adults in Aizu cohort study (LOHAS). Scientific Reports, 12(1). https://doi.org/10.1038/s41598
022-15173-y
Raja, A., Hoang, S., Patel, P., & Mesfin, F. B. (2022, July 17). Spinal Stenosis. StatPearls – NCBI Bookshelf.
https://www.ncbi.nlm.nih.gov/books/NBK441989/
Ruggiero, E., Bonaccio, M., Costanzo, S., Esposito, S., Di Castelnuovo, A., Carpineta, E., Cerletti, C.,
Donati, M. B., Paolini, S., Esposito, V., De Gaetano, G., Innocenzi, G., Iacoviello, L., Investigators, P.,
Investigators, P., Staff, R., Biobank, & Analyses, B. (2022). Dietary factors and the risk of lumbar spinal
stenosis: A case–control analysis from the PREFACE study. Nutrition Metabolism and Cardiovascular
Diseases, 32(1), 90–97. https://doi.org/10.1016/j.numecd.2021.09.019
TeachMeAnatomy. (2022, November 14). The Vertebral Column – Joints – Vertebrae – Vertebral Structure.
https://teachmeanatomy.info/back/bones/vertebral-column/
Wan, B., Ma, N., & Lu, W. (2023). Evaluating the causal relationship between five modifiable factors and
the risk of spinal stenosis: a multivariable Mendelian randomization analysis. PeerJ, 11, e15087.
https://doi.org/10.7717/peerj.15087

